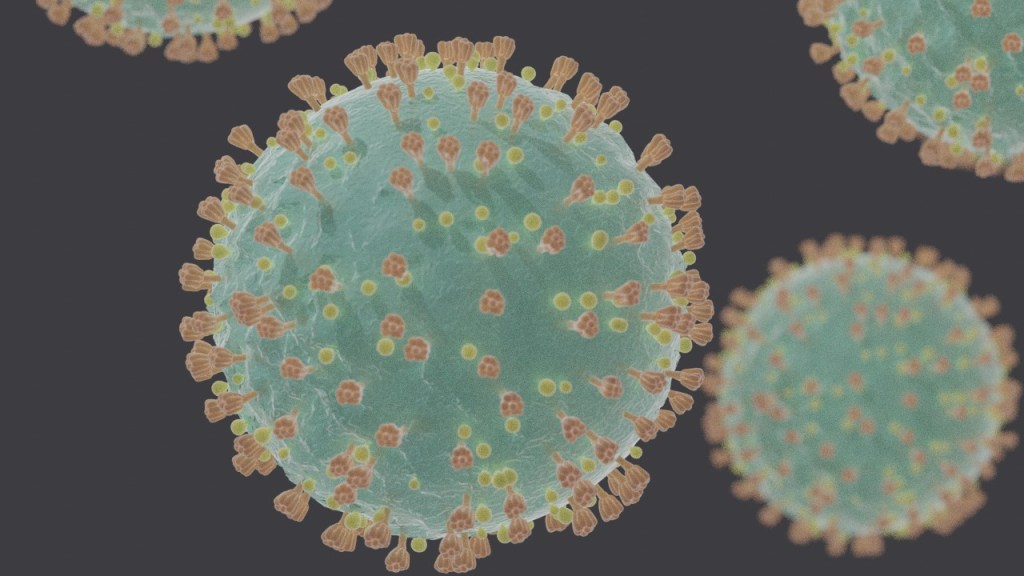
As I write we are in the midst of a world-wide epidemic on a scale unprecedented in modern times. What we know about the virus and the epidemic is shifting at such a pace that it’s only by watching key websites and following the news that you can keep up.
This blog is no substitute for that. It just fills in some of the scientific terminology and key concepts. The main scientific topics seem to me to be: viruses, lungs, vaccines, epidemics and social behaviour. As I am not a specialist in any of these fields, let me know if you spot an error. Here we go!
Viruses
The image above is a representation of a few viruses that cause the COVID-19 disease, generated by a computer from a photograph taken under an electron microscope – a very high magnification microscope. This virus caused the outbreak of respiratory illness first detected in Wuhan, China in 2019. The illness has been named coronavirus disease 2019 (COVID-19). The virus that causes it is named SARS-COV-19 to reflect it’s similarity to the related coronavirus that caused the earlier SARS outbreak (Severe Acute Respiratory Syndrome)
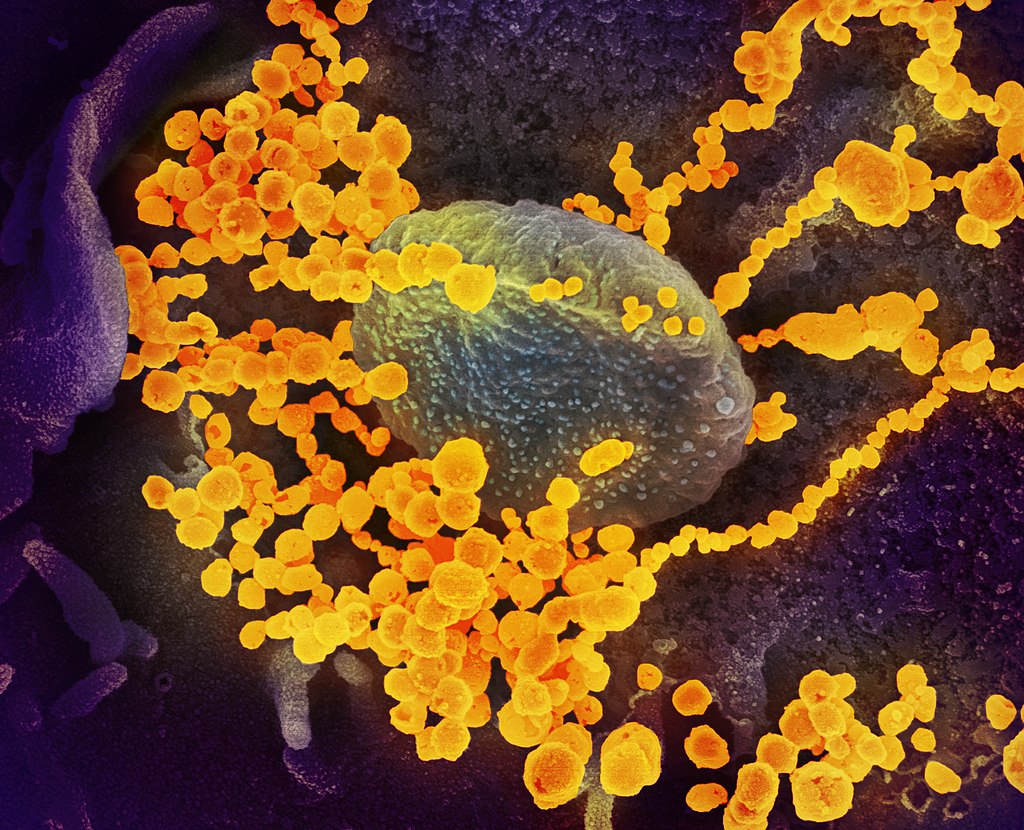
This image was isolated from a patient in the U.S.A. It was taken through an extremely high powered microscope, known as a scanning electron microscope and shows multiple copies of the virus (round gold objects) surrounding an intact cell (rugby ball shape in the centre) cultured in the lab. Although the precise position and shape of the cell from the which the viruses are emerging is not clear, it is easy to see that viruses are much smaller things than cells.
The corona virus is roughly 100 times smaller than a cell[i]. Strange though it may seem, it’s an open question whether a virus is a living thing or not. It depends on your definition of “living”. Virologists describe them as leading “a kind of borrowed life.”[ii] This ambiguity arises because they are unable reproduce themselves; they rely on breaking into living cells and commandeering their machinery. This is why they are so dangerous: the cells they enter are destroyed in the process.
This diagram of a coronavirus (not COVID-19 specifically) shows the basic architecture of a virus:
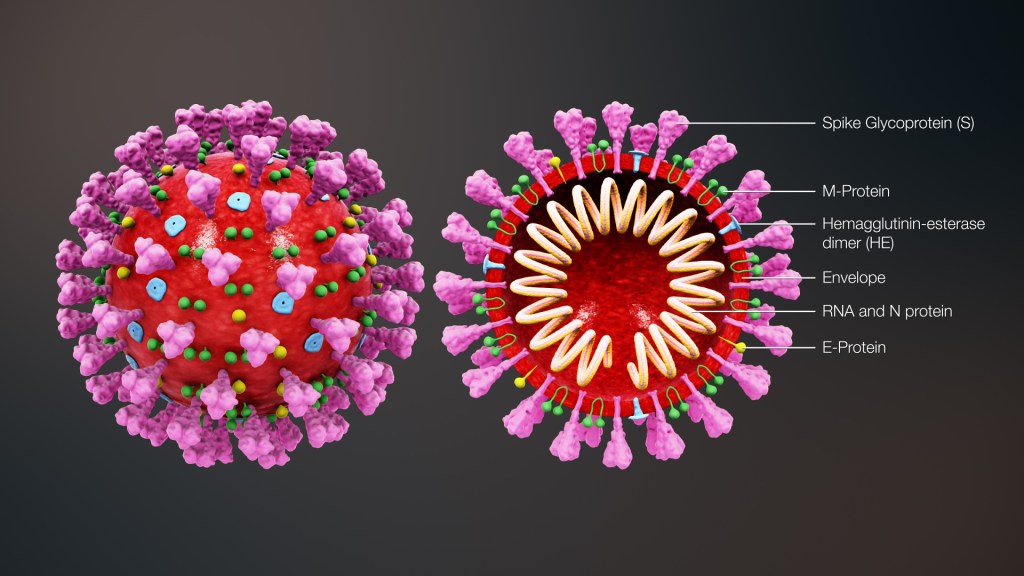
It’s an amazing assembly of large and giant molecules – an extraordinary piece of engineering. On the left you can see it’s outer shape – a sphere in this case, but quite different in other cases. The red coloured surface (envelope) is made of oily molecules (lipids) and is studded with various types of protein molecule that penetrate through to the interior. It’s this oily envelope that soap is able to break up when hand washing. Just a few weeks ago (19th February 2020), the big pink protein, called spike glycoprotein S was identified by a team at the University of Texas[iii] as the key molecule that locks on to cells in the lungs. A reader in Malaysia, who is a glycoprotein scientist, points out that unfortunately this ‘spike’ molecule is different from that of its predecessor SARS-CoV-1. This means the same vaccine and antiviral drug approaches may not necessarily work for COVID-19.
The envelope is a protective container inside which lies the blueprint for making more viruses – the RNA. This is very similar to DNA and serves the same function, providing the vital genetic information for the production of new viruses. What a virus does not contain however is the machinery to use this blueprint to reproduce itself. Instead it breaks through the outer surface of living cells, much larger than itself, and uses their machinery to reproduce its RNA rather than the cell’s own DNA. It’s a freeloader!
COVID-19 is a specific, recently mutated version of a coronavirus. The coronavirus family is very familiar to virologists as its various members are associated with the common cold, as well as more severe disease such as Middle East respiratory syndrome (MERS) and Severe Acute Respiratory Syndrome (SARS).
Lungs
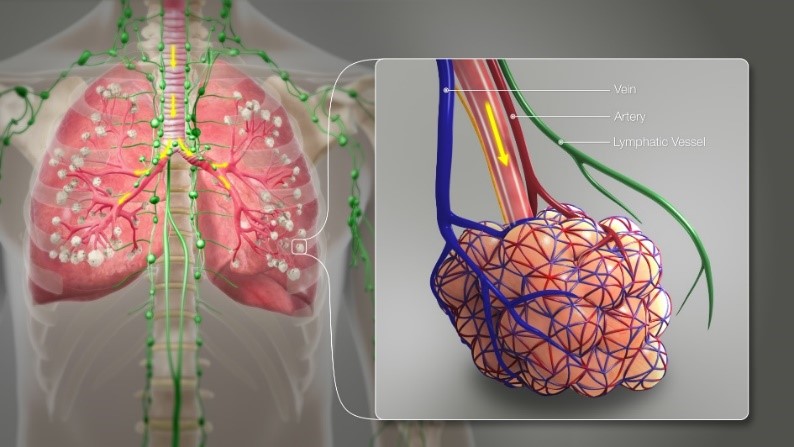
Lungs are the particular organs in the body that contain the specific type of cells the virus latches on to. This diagram shows the airways of the lung branching out across the lungs from the central windpipe (trachea).
The tip of one of the smallest branches is enlarged to show how the cavity containing air you breathe in is surrounded by tiny blood vessels. This is where oxygen passes from the airways into the arteries (red) and carbon dioxide passes out the other way from the veins. The cells that line this cavity, are the target for the coronavirus. Like the virus itself, these cells also have protein molecules projecting out of their surface. The fatal interaction occurs when the protein sticking out of the virus “matches” the protein sticking out of the cell.
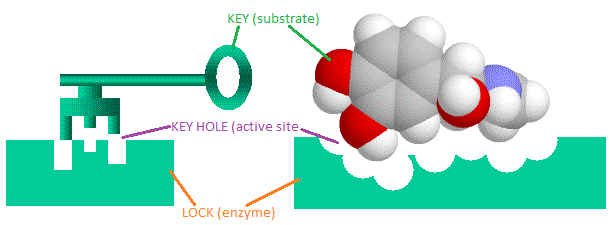
“Matching” here means that the protein on the virus has complementary features to those on the cell; rather as a key has a complementary shape to the lock into which it fits.
A few weeks ago, on 4th March 2020, a team at Westlake University in Hangzhou identified the structure of the receptor protein on the surfaces of the respiratory cells and worked out how it interacts with the protein on the surface of the virus.[iv] Knowing the structure of the key (the virus protein ) and the lock (the protein in the lung cells) could theoretically be a starting point for developing drugs. In principle, pharmacological research proceeds on two fronts: first, looking for vaccine; second look for an antiviral drug. The “spike “ protein on the surface of the virus could be a promising target for a vaccine. It is likely this could be developed over the coming year. It would stimulate the immune system to destroy viruses emerging from infected cells.
One of our readers sent this link to a very well-made animation video that explains very clearly the whole process of the disease, its spread and how we can slow it.
Drug development
Finding a drug that prevents a virus entering a cell in the first place, by damaging it or preventing it reproducing, would be “new territory”, according to a virologist at Loyola University in Chicago. Antiviral drugs are proving hard to develop because of the risk of damaging the very cells the virus is entering. Some, such as aciclovir (Zovirax) for herpes are nevertheless emerging.
However, an alternative route is to see whether drugs already proven to be effective might also work against the COVID-19 virus. The advantage of “re-purposing” existing drugs is that they will have already been tested for safety, toxicity and ability to remain intact in the body. This shortens the time needed for trials. News has just broken of trials of just such a drug, known as Favilavir or Avigen[v]. It was approved in China On March 15, 2020 for the treatment of influenza and also for use in clinical trials for CPVOD-19. One week later, on 22 March, Italy approved the drug for experimental use against COVID-19 and began conducting trials. But, as the Italian Pharmaceutical Agency reminded the public, existing evidence in support of this drug is scant and preliminary.
Vaccines
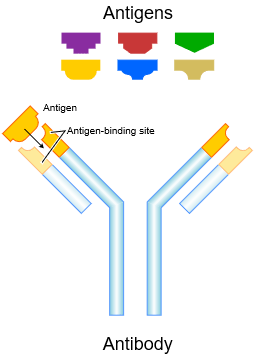
A vaccine works by provoking the immune system to produce antibodies to an unwanted substance in the body. The vaccine consists of some disabled fragment of the offending molecule (known as an antigen) – for example, it may just be part of one of the protein molecules on the outer surface of the virus. This can be sufficient to trick the immune system into developing antibodies to the virus. Antibodies are giant protein molecules, produced in specialised cells of the immune system, which attach to the alien molecules and signal to the body’s defences that they are to be disposed of.
Thus, scientists across the world will be working overtime to find some kind of fragment or disabled version of the “spike” protein on the surface of the virus that will provoke the body to produce antibodies to it. This would be injected into our bodies when we are vaccinated. The immune system easily fights off this fragment but, crucially, it also “remembers” it by keeping copies of the antibodies that did this. If the real virus should subsequently present itself these “archive” copies are used to mass-produce the appropriate antibodies quickly, on a huge scale. These then go on to eliminate the viruses.
That’s how vaccines work. But it’s no easy task developing a practicable vaccine: it has to be proven to be safe as well as effective. The U.S. Centers for Disease Control and Prevention consider that the earliest one could be available is in a year to a year and a half.
Part 2 of this extended blog will follow shortly. It explores some of the scientific ideas about epidemics and social behaviour.
© Andrew Morris 24th March 2020
Read more
According to the UK Government website[vi], coronaviruses are a large family of viruses with some causing less-severe disease, such as the common cold, and others causing more severe disease such as Middle East respiratory syndrome (MERS) and Severe Acute Respiratory Syndrome (SARS) coronaviruses.
According to a very readable National Geographic article[vii], early data on COVID-19 shows that about 82 percent of cases have milder symptoms. In previous SARS infections, particular lung cells called cilia get destroyed and fill the airways with debris and fluid. The immune system clears away the damage but sometimes it overreacts, killing healthy cells and adding to the debris. That’s when people have to be put on ventilators.
The Live science website[viii] has useful and readable information about the disease. Amongst other things, it tells us that coronaviruses we know about “generally cannot survive for more than a few hours on surfaces outside a human host”, but, according to the US National Center for Immunization and Respiratory Diseases, “scientists don’t yet know how long the novel coronavirus can survive outside a host”.
Links to sources
i. A typical cell is around 12 micrometres – around 5 – 10 would fit across a human hair. Coronavirus is about 0.12 micrometres across
ii. https://www.scientificamerican.com/article/are-viruses-alive-2004/
iii https://www.livescience.com/how-coronavirus-infects-cells.html
iv https://www.livescience.com/how-coronavirus-infects-cells.html
v https://en.wikipedia.org/wiki/Favipiravir
vii https://www.nationalgeographic.co.uk/science-and-technology/2020/02/heres-what-coronavirus-does-body
viii https://www.livescience.com/what-are-coronaviruses.html
