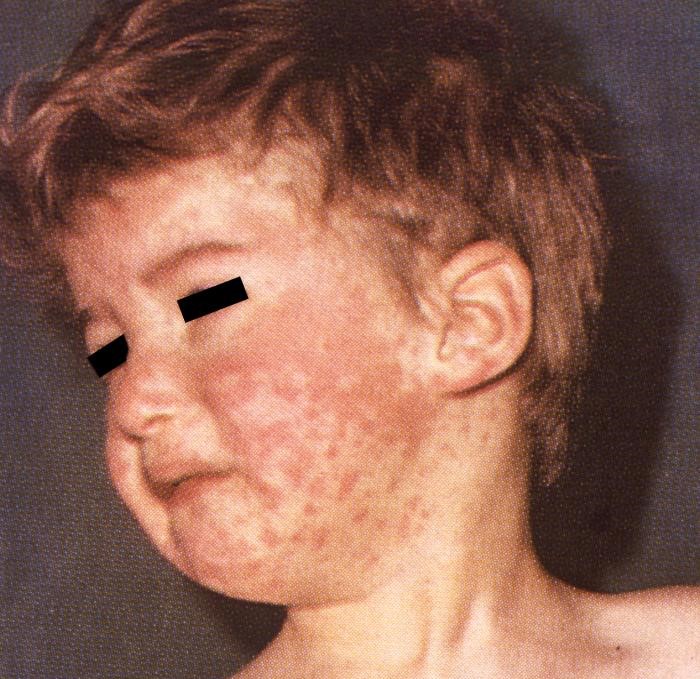
What’s driving the anti-vaccination trend? This question was raised in a science group discussion as the media were reporting a dangerous rise in measles, once believed to have been eradicated in the UK. The increasing popularity of conspiracy theories seemed to be one explanation – vaccination by ‘the authorities’ being perceived as a plot by some people.
The pro-vaccination argument was expressed by a grandmother in the group, worried about her grandson, who, while too young for his MMR injection, had developed a rash of red spots. The moral question arose: was it acceptable for parents to refuse the MMR vaccine yet allow their children to mix with others too young to be vaccinated. Someone in the group recalled a time when parents would organise “chickenpox parties” to ensure their children got exposed early to the virus in order to develop immunity.
From these social and moral concerns basic questions emerged: what exactly is meant by immunity? What does vaccination involve? How does your body remember that it once had measles? How is the body able to protect itself, not just against measles, but all the other possible diseases? We may understand broadly that the immune system protects you against germs and that vaccination involves putting small harmless bits of a disease into you in order to create antibodies. But what exactly are antibodies?
The immune system does indeed protect you, and it targets more than just germs: it works against anything it recognises as not belonging to the individual. As we know, it can even work against the body, when it tries to reject a transplant for instance, or overreacts to pollen or cat fur in an allergic reaction. As a “system” the immune response is not located in a single place but is distributed throughout the body. Nor does it act in a simple single manner: there are several components in the system. The two main strands are the antibodies that we have already mentioned and the white blood cells (or leukocytes – ancient Greek for “white cells”). These two function quite differently and are on quite different scales. Antibodies are molecules (very large ones) whereas leukocytes are cells made up of many and varied types of molecule – roughly 1000 times larger than an antibody molecule. In this blog we focus on antibodies.
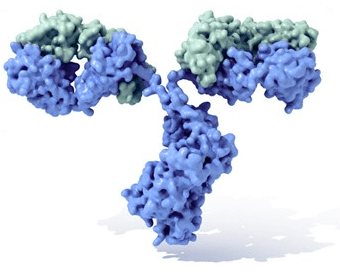
Antibodies are molecules that are manufactured and stored inside white blood cells – a specialised type called a B cell. They are protein molecules, as are a huge variety of other types of chemical in the body, including all enzymes, some hormones and vital components of muscle, ligament, hair and blood.
Antibody or “immunoglobulin (courtesy of the US National Library of Medicine). In the image , the blobs represent atoms.
Antibodies are a type of protein molecules – but they are truly gigantic ones. You could say they have to be huge, as they have to come in thousands of slightly different varieties in order to recognise and protect us against the vast range of potential threats.
One strain of antibody counters the measles virus, another mumps, another rejects an alien heart transplant and another sets off an allergic reaction to peanuts.
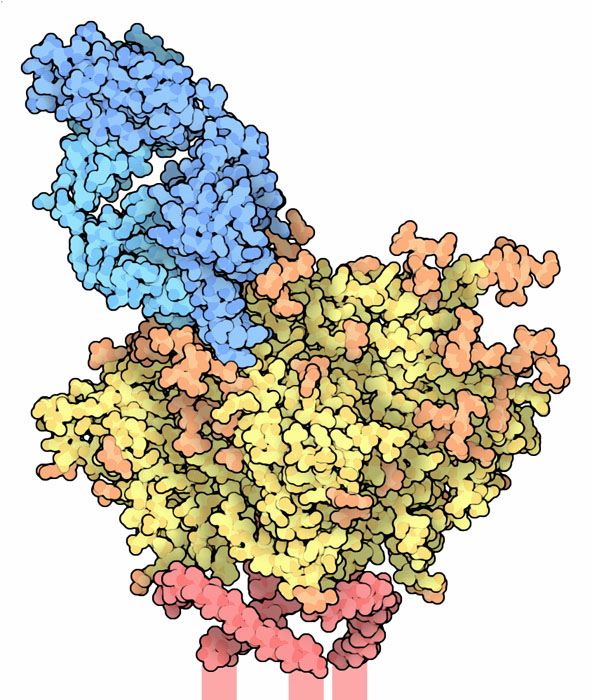
So, different antibodies need to be sufficiently similar to one another to ensure they are all capable of disposing of unwanted bugs, but at the same time sufficiently distinct for them to respond to each of the many potential threats. Their unique Y-shaped structure makes this amazing feat possible.
The model opposite shows part of an antibody in blue attached to an antigen from surface of an HIV virus (yellow, orange and red)
But how does your immune system protect you against all manner of diseases – how does it recognise them all? Does it have templates ready to produce exactly the right antibodies for any germs just when they are needed?
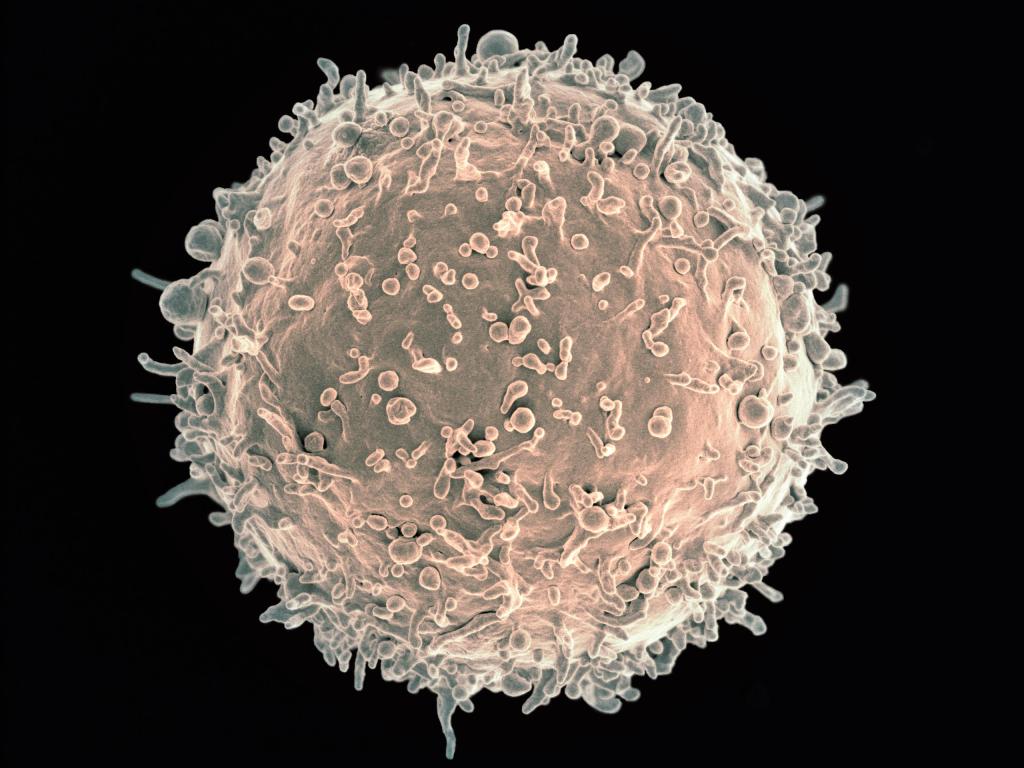
Research has revealed that once an antibody has been produced for the first time, say against the measles virus, copies of it remain stored in specialised memory cells (a type of B cell) indefinitely. Copies of it are also held on the outer surface of the same cell where it acts as a receptor.
Human B cell (Image courtesy of the US National Institute of Allergy and Infectious Diseases )
If that particular antigen (say a protein on the surface of a measles virus) enters the body ever again, it is recognised by the receptor on the surface and this triggers these specific cells to multiply massively, thus releasing large amounts of just the right antibody into the bloodstream.
That’s why you don’t get infections such as measles twice. It is also why vaccines are needed early in life, to provoke the body into producing antibodies safely, before the offending bug causes an unpleasant or dangerous illness. In this sense you acquire the capacity to generate antibodies to specific threats through previous experience – the immune system ‘learns’ and remembers. Anyone who has suffered ‘flu repeatedly knows that it doesn’t always work out quite like this, particularly if a virus mutates and evolves from year to year.
For the antibody molecule to identify an unwanted bug and then combine with it is the important first step in combatting disease; but what happens next – how does your body then get rid of it? As with many of the systems in our highly evolved bodies, there are several ways. In the simplest of these, a host of antibodies simply cover the surface of the invading bug and neutralise it, prevent it functioning. Another way is for several antibody molecules to link together, or “agglutinate”, several bugs and thus incapacitate them… and there are other ways too.
These neutralised bugs or agglutinated clusters then get spotted by one of the many types of white blood cell which hang about watchfully in connective tissue, called macrophages. These cells simply engulf the offending material, ingest it and remove it from the body.
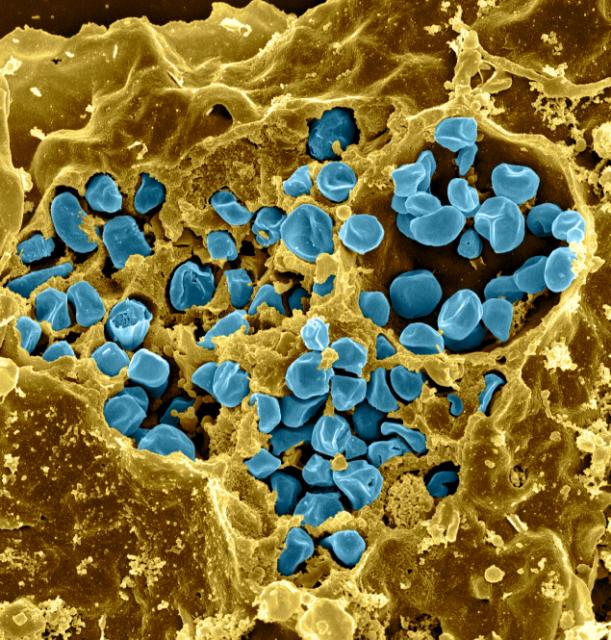
This photograph taken with a very powerful microscope shows a macrophage (gold colour) that has engulfed unwanted material, in this case, an ulcer-forming bacterium (blue). (Image courtesy of the US National Institute of Allergy and Infectious Diseases)
It’s important to emphasise that this story of the role of antibodies in combatting disease is only one aspect of the body’s many-stranded defence system. Apart from antibodies the body also defends itself through physical barriers, such as the layers of the skin, through the action of specialised chemicals and through cells that identify and ingest unwanted guests.
So far we’ve considered the vital role the antibody system plays in combatting bacteria, viruses and other unwanted beasties that enter our bodies. Unfortunately the same system is also capable of working against our best interests on occasions. Those who suffer from hay fever or other allergies know that some antigens, found for example in cat fur or hay fields are capable of triggering an immune response causing eyes to water, noses to run and tissues to swell. Others suffering with rheumatoid arthritis know what it feels like for the immune system to attack the body’s own tissues, in this case, in the joints. And anyone benefiting from a transplant knows that their precious immune system has to be suppressed artificially in order to prevent the imported organ, with its alien antigens, being rejected.
The intricacies of allergic reactions and autoimmune conditions will, no doubt, be of interest to many people, so perhaps we’ll make this the main focus of a future blog.
© Andrew Morris 29th September 2019
