
By the summer of 2022 the Covid virus had morphed into something even more catchy. Friends and colleagues everywhere succumbed, including many who’d evaded it up till then. Fortunately symptoms seemed to be relatively mild and, apparently, much the same for different people. During a science discussion, Patrick, who was still recovering from the infection, reported slight back ache and a foggy head and, unusually for him, a feeling of listlessness. He’d lost interest in doing the things he usually enjoyed – reading, listening to music , seeing people.
Figure 1 Boy with a cold.
His motivation, his mojo had just gone. Jean described a similar feeling after a bout of flu some years ago: “ I lost any expectation that I could do anything. I just flopped about in and out of sleep, half listening to snatches of radio”. Julie commented that these seemed like classic symptoms of depression.
Losing motivation through illness makes you wonder how it is that you ever feel a sense of purpose under normal conditions. What is it that makes us want to get on and do things? Why do we lose this desire when we feel ill? Come to think of it, what actually is illness?
Illness
We know from the Covid experience that an infection can have very different consequences for different individuals. For some it may mean just a feeling of being “off colour”; for an unfortunate few it may mean whole organs, like the lungs, become seriously, perhaps fatally, damaged. What’s the difference between an unpleasant feeling and a serious assault on your body?
An article in the British Medical Journal draws a helpful distinction between different concepts and vocabulary for being unwell. It suggests that:
- illness is a feeling, entirely personal to the patient which often accompanies disease.
- disease is a pathological process, a deviation from a biological norm which doctors are able to see, touch, measure, smell.
- sickness is a social role, a bargain struck between a person and society that supports them
Illness, rather than disease, is usually how laypeople think about being unwell: it’s a personal feeling, a set of symptoms. Conversations with friends and colleagues about the effects of Covid-19 infection seem to bring out a broadly common set of symptoms: fatigue or ‘lack of energy’, ‘brain fog’, aches and pains in various places, for example. (At the time of writing, July 2022, omicron variants BA 4 and 5 are the dominant strains). The medical profession has adopted the French word “malaise “ to describe this condition.
A live research project in the UK, called the ZOE Symptom Tracker, kept abreast of the reported symptoms of several million volunteers on a daily basis throughout 2020 and 2021. The most common symptoms varied to some extent over the course of the pandemic, perhaps reflecting the differing effects of the evolving variants. Initially ‘loss of taste’ was significant, later less so, as ‘runny nose’ became more common. Respondents were describing their illness, as they experienced it, on a daily basis via an app. It is remarkable how consistent these self-reported accounts were, from day to day and week to week, thanks to the huge sample size. The symptom list surely helped people diagnose themselves in addition to its primary purpose in providing epidemiological data.
To move beyond the ‘illness’ – the subjective feelings associated with the symptoms – to an understanding of the underlying disease, we need to explore in greater depth the causes of the symptoms. Why do our noses run, our heads ache, our energy levels flag? Why is our body responding to the virus in the way it does? A runny nose, the most mundane of symptoms, makes a good starting point.
A key function of our noses, even on a good day, is to trap unwanted particles and bugs that we may breathe in. It achieves this thanks to a layer of sticky mucus lining the nostrils (and the rest of the respiratory tract) which is continuously swept upwards along the nose (Figure 2).
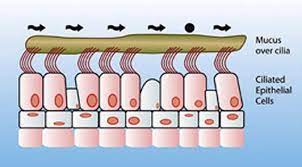
Figure 2 removing unwanted particles in the nose

This disposes of the unwanted material trapped in the mucus via the mouth and digestive system, ensuring our lungs are protected from it. Tiny whip-like protrusions on the cells lining the nostrils, known as cilia, carry out the continuous sweeping function.
Figure 3 close-up cilia
With infection, however, this waste disposal system goes into overdrive. Once the immune system detects an infectious bug it responds in multiple ways to obstruct its progress. One way it achieves this is by sending out messenger chemicals called cytokines which turn up mucus production in cells in the lining of the nose (amongst other things). This helps to move the offending, trapped particles along more effectively. It also leads to inflammation: your nasal lining swells and fills with fluid to ensure the cytokines reach everywhere. That’s a runny nose. The immune system is working to eliminate the offending particle or bug.
The immune response
It turns out that it’s not just a runny nose that the immune system is responsible for, it’s most of the feelings associated with being ill. Much of ‘feeling ill’ is, surprisingly not a direct effect of the invading pathogen but of our body’s response to it. When the immune system is activated by an unfamiliar bug or molecule it releases a range of chemicals which cause diverse changes to tackle the invasion.
The term ‘inflammation’ (meaning ‘set on fire’ originally) is used to describe the suite of effects caused by the response of the immune system. For Latinists, these are captured in four rhyming words dating back to Roman medicine: rubor, calor, tumor and dolor. They refer, respectively, to redness, heat, swelling and pain. These cover the all-too-familiar effects of any inflammation: head cold, fingernail splinter or larynx. The tissue swells up, reddens then becomes hot and tender.
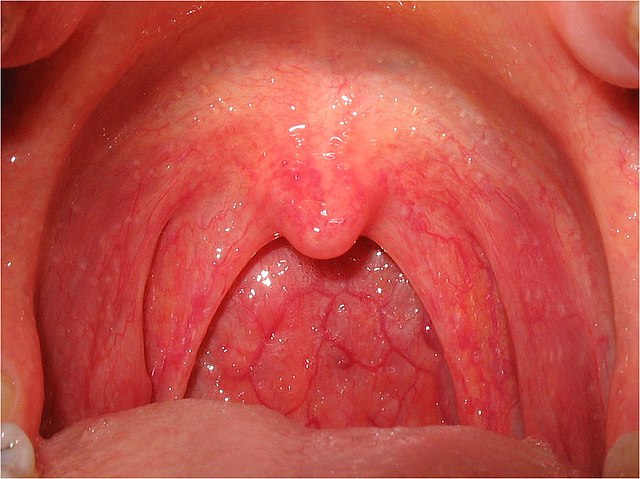
Figure 4 inflamed larynx
These are all beneficial effects stimulated by the chemicals released into the blood by the immune system. Arriving at the scene of infection or injury, some of these cause the blood vessels to dilate, increasing the blood flow. This delivers materials to the site more rapidly, reddening the surrounding tissue in the process. Other chemicals make the walls of the blood vessels permeable, allowing fluid to ooze out into the surrounding tissue, delivering helpful molecules to the exact spot required. This causes the tissue to swell up. Others still, activate pain receptors on nerve cells, signalling to the brain the site of distress and alerting the poor sufferer to the danger. It’s not difficult to see how these responses account for several of the general symptoms of illness. Aches and pains simply result from the inflammation brought about by the immune system. So do local swellings and feeling hot. But what about the other, subtler, but no less debilitating effects we feel: listlessness, lack of energy, fatigue? How are these accounted for?
Cause of fatigue
Fatigue is a feature of many conditions, both temporary (acute) and longer term (chronic). It is felt particularly by people living with conditions such as multiple sclerosis (MS), Parkinson’s and Myalgic Encephalomyelitis (ME). The causes of fatigue are not well understood, but in some conditions seem to be linked to inflammation. It may be that in the case of Covid-19 and other infections, fatigue is a consequence of the immune response. It is distinct from tiredness which is resolved by sleep and is different from a physical lack of energy. One line of research is suggesting that it may be the result of interference in the way we develop the motivation to do things. The cytokine chemicals mentioned above, that are released during the inflammation process, appear to bring about changes within the brain. Amongst other things, these alter the way the chemical dopamine is made and used there, reducing its effectiveness. This change brings about fatigue, weakening of the sense of pleasure, and slowing down of body movements. Dopamine is a neurotransmitter: one of several chemicals that enable communication between nerve cells. As part of the reward system in your brain, it plays a key role in the neuronal pathway that gives us a sense of pleasure and the motivation to do things.
Philosophically, the discussion group found it odd to think in such a biochemical way about things that are so subjective, so close to our very sense of purpose in life. Recalling her bout of flu, Jean said: “surely you just lack energy when you’re ill because its diverted to fight off infection?” Yet, it’s a reality that specific aspects of our feelings and behaviour do correspond to particular chemical changes in the brain. Studies that look for such associations are at the heart of research into Alzheimer’s, Parkinson’s and other brain disorders. Some types of research look for an excess or deficiency of a particular chemical in the brains of individuals exhibiting distinctive kinds of behaviour. Other types analyse behavioural trends in people (or animals) with injuries to specific part of the brain or the effects of electrically stimulating precise locations in the brain. These plain facts force us to think about the extent to which we can be said to act freely as a result of our will, or are simply pushed by our biochemistry. Views differ on this philosophical point!
These considerations about the link between your chemistry and your feelings led Jean, Patrick and Julie in a discussion session to turn their attention away from illness towards its opposite: normal health. If the feeling of everyday wellbeing can be compromised at the drop of a hat, what is it that keeps you going under normal circumstances? We now know that a virus can get into your system and activate an immune response, which brings down your mood and makes you feel listless and fatigued. So how can we describe what it is that gets lost when this happens – what do we mean by our spirit or energy, joie de vivre or mojo? As part of their illnesses, Patrick and Jean had both felt a distinct loss of interest in the things they usually enjoyed doing: reading a book, meeting up with people or listening to music. What is it that gives us the sense that things are worth doing, under normal circumstances?
Motivation
Psychologists describe this aspect of human behaviour in terms of motivation. As you might expect there are various theoretical models of what causes us to act as we do. Some focus on the drive to satisfy primary needs, such as hunger and thirst, others emphasise the role of curiosity and play, others, social rewards. Studies in which animals are deprived of stimulus in various ways, reinforce the importance of a stimulating environment in maintaining positive mood. Experiments in which humans are deprived of sensory inputs lead to psychological discomfort and potentially, hallucinations. Rats trained to use a maze will spend extra time exploring it, if something is changed in it. Monkeys persist in tackling physical puzzles presented to them even when there is no simple reward for doing so, such as food: a sign of instinctive curiosity.
Of course, psychology experiments often use simple rewards such as food to study the generic system in animals. Patrick wondered how widely the concept can be applied to the real lives of human beings (and indeed other higher animals). Psychologists use the idea of ‘reward’ widely, to include, for example: receiving praise, gaining social recognition, advancing our careers, establishing relationships acting altruistically as well as the more obvious other aspects of our everyday behaviour.
What these various theories coalesce around is the concept of ‘motivation’ to describe what makes us behave in purposeful, goal-directed ways. Clearly some fundamental actions are driven by basic necessities such as food and sleep, others however are driven by expectation of a reward. Indeed, specific areas of the brains have been identified as ‘reward centres’ in research on rats. When trained to press a lever that stimulates a reward centre, they do so repeatedly to excess, even overriding their urge to eat or drink.
How humans and other animals behave in various experimental situations is the work of experimental psychologists. They observe behavioural results under differing conditions, enabling conclusions to be drawn about abstract concepts such as motivation. To find out what is happening physiologically within the body – especially the nervous and hormonal systems – under such conditions is the work of neuroscientists. Their studies reveal that the ‘reward system’ inferred from behavioural studies is embodied in an interconnected set of structures in the brain with neuron pathways linking them. More specifically they implicate the chemical dopamine when animals engage in activity that is naturally rewarding, such as eating. It is released when we expect to receive a reward and is involved in the emotion and memory systems associated with rewards.
Mechanism of fatigue
So we now understand fatigue as the result of interference in the brain’s reward system, thereby lowering our motivation. But how is it that an objective process – weakening in particular chemical pathways – dopamine in particular – gives rise to the subjective feeling of fatigue? Fatigue researchers are investigating several alternatives explanations for this.
One possibility centres around the body’s ability to know about itself. Unconscious of it though we are, our brains are continually monitoring where our limbs are, what our blood temperature is and many other bodily states. They stand ready to act if they detect any significant deviation from the norm. The proposal is that fatigue is a representation of the brain’s loss of control and lack of a course of action. The feeling of fatigue would be the sense that nothing can be done. An alternative suggestion is that the feeling of fatigue results from an error or surprise – some kind of mismatch between expectations by the body’s self-monitoring system and what is actually happening. A third mechanism proposed is that the sense of fatigue comes from errors occurring in the body’s monitoring and prediction of movement – known as the proprioceptive system. In this scenario, the brain is misled into expecting that physical movements require more effort than they actually do. In this view, fatigue is not so much an actual lack of energy but an exaggerated perception of effort required.
This new idea of fatigue, as a kind of perceptual error rather than an actual lack of energy, led the discussion group to consider the obvious next questions: “what do we mean when we talk about “energy” in the bodily sense? What are tiredness and sleep all about? If you have the energy, you can read about this in the Further Reading section below.
Conclusion
In summary, the sense of exhaustion, tiredness or low energy that may accompany illness, depression, poor diet, disturbed sleep or excess use of toxic substances may have both a physical energy component – lack of glucose – but also a perceptual component. The latter may be a response by your brain, activated by the immune system, to bring about a sense of fatigue and loss of motivation, serving to keep you at rest and away from social contact. So next time we feel low as part of an illness, maybe we should just take it on the chin, dismiss our gloomy thoughts and remember our bodies are doing their best to get us through the raging infection.
© Andrew Morris 17th August 2022
If you’ve still got the energy, a discussion of why evolution may have given rise to the fatigue process is given in the Further Reading section below.
Further reading
Sleep, tiredness and energy
It’s easy to slip into an oversimplified idea that sleep follows from tiredness, like refilling a petrol tank when it’s empty. In fact the urge to sleep is influenced by several different factors, not just level of energy. At the top level, the universal rhythm of day and night, with its associated light levels, sets a kind of bodily timer. This so-called circadian (i.e. 24 hour) rhythm regulates the release of hormones throughout the night, in particular melatonin is strongly associated with sleep. Sleep itself not only reduces demand for energy, but also helps clear toxins, replenish stocks of the energy molecule ATP and, through dreaming, process mental experiences during the day[ix].
Many factors have been found to influence the feeling of tiredness . The UK National Health Service cites, for example: psychological causes such as stress, anxiety and depression; physical causes such as iron deficiency, underactive thyroid and disturbed sleep; lifestyle issues, such as shift working and caffeine consumption and particular conditions, such as obesity, pregnancy and cancer. Many of these will be familiar to each of us.
Energy is a word used loosely in everyday conversation as the basis for feelings of liveliness, alertness and physical fitness. The vagueness of the concept has encouraged a massive industry to develop, offering drinks, foods and medicinal supplements purporting to restore energy levels. Scientists avoid this usage, preferring instead the concept of fatigue to describe the absence of liveliness. Energy on the other hand does have a clear scientific meaning .Strictly speaking it is defined in physics as “the capacity to do work” – where “work” is the result of a force moving through a distance.
The way energy, in this stricter sense, is used in living bodies is relatively well understood today. Foods are made of large molecules within which energy is locked up, much like the energy in a coiled-up spring. Digestion breaks these up, and, in the case of carbohydrates, releases the smaller glucose molecules of which they are made into the blood stream. Passing into all our cells, these smaller molecules offload their energy and in a complicated set of chemical steps makes it available, via a universal molecule called ATP, for delivery wherever it’s needed: to contract muscles, activate brain cells, maintain body temperature or act in countless other ways.
Chemical energy derived from foods (mainly carbohydrates and fats) is essential for maintaining all bodily processes, including mental ones. Lack of energy in this more strict sense is clearly debilitating in a great variety of ways. It reduces the power of your muscles, impairs your thinking and slows down the rate of chemical processes in cells everywhere. No wonder you feel low when deprived of food!
Evolution of the fatigue process
In summary we now know, thanks to decades of research using various kinds of intervention with different animals, that our brains – and those of other animals – are equipped with biochemical processes that induce us to make efforts in order to gain a reward. Being purposeful or working towards a goal brings us a reward. Distinct ‘pleasure centres’ have been identified in the brain that foster reward-seeking behaviour. One possible explanation of fatigue as a symptom is that it corresponds to an alteration in the reward system, lowering dopamine levels and, as a consequence, motivation. In other words, we feel listless when we are unwell, lacking the will to do things we normally enjoy, because our brains are making us be like this.
It is this lack of motivation that explains the sense of fatigue rather than any actual lack of physical energy. So, why on earth do we get into such a state when we are ill – “what’s the point of fatigue?”, as Jean put it in the discussion. One answer to this has been suggested by neuroimmunologists in Israel’s Weizmann Institute: perhaps this unwell feeling was an evolutionary adaptation. The hypothesis is, that by feeling fatigued you get around less to infect others and you lose interest in eating and other social activities. The net effect is that you are less likely to pass an infection on to those around you – mainly kith and kin in primitive societies. Even if you were to die, your genes, embodied in those of your near relatives, would have been spared. Genes closely linked to yours would live to be perpetuated in future generations .This is an example of the “selfish gene” idea that evolution ensures the survival of genes rather than the individual carrying them.
© Andrew Morris 17th August 2022
